Cognitive Behavioral Therapy (CBT) A Practical Guide
Cognitive behavioral therapy (CBT) offers a powerful approach to understanding and managing a wide range of mental health challenges. This evidence-based therapy focuses on the interconnectedness of thoughts, feelings, and behaviors, providing individuals with practical tools to identify and modify unhelpful patterns. From managing anxiety and depression to overcoming addiction and fostering resilience, CBT empowers individuals to take an active role in their mental well-being, fostering lasting positive change.
By exploring the core principles of CBT, its various techniques, and its applications in diverse contexts, this guide aims to provide a comprehensive overview of this transformative therapeutic approach. We will delve into the practical application of CBT strategies, examine its integration with mindfulness practices, and explore its role in promoting mental health advocacy and personal growth. The journey through this guide will equip you with a foundational understanding of CBT’s potential to improve mental and emotional well-being.
Introduction to Cognitive Behavioral Therapy (CBT)
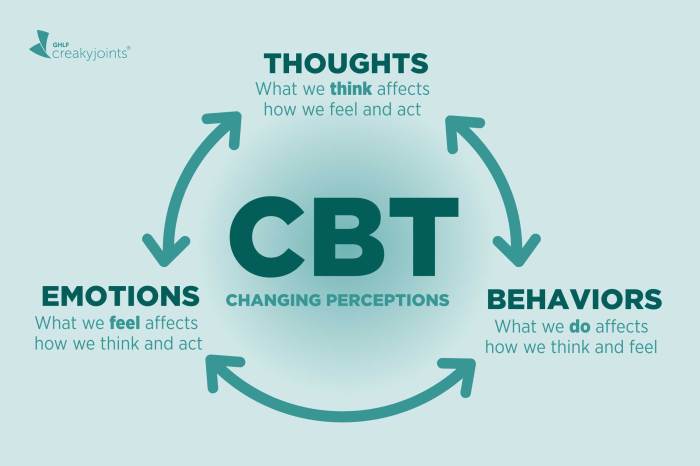
Cognitive Behavioral Therapy (CBT) is a widely-used, evidence-based approach to psychotherapy that focuses on the interconnectedness of thoughts, feelings, and behaviors. It operates on the principle that our thoughts significantly influence our emotions and actions, and by modifying unhelpful thought patterns, we can improve our emotional well-being and behavior. This approach emphasizes practical skills and techniques to help individuals manage and overcome various mental health challenges.CBT’s theoretical underpinnings are rooted in cognitive psychology and behavioral learning theories.
Cognitive psychology explores how our mental processes—such as perception, memory, and thinking—shape our experiences. Behavioral learning theories, such as classical and operant conditioning, highlight how learning and environmental factors influence our behaviors. CBT integrates these perspectives, suggesting that maladaptive behaviors are often learned and maintained through cognitive distortions and reinforcement patterns.
The History and Evolution of CBT
CBT’s origins can be traced back to the work of several influential figures in the mid-20th century. Aaron Beck’s work on cognitive therapy in the 1960s, focusing on identifying and challenging negative automatic thoughts, laid a crucial foundation. Simultaneously, Albert Ellis developed Rational Emotive Behavior Therapy (REBT), emphasizing the role of irrational beliefs in emotional distress. These early approaches gradually evolved, integrating elements of behavioral techniques, leading to the development of the comprehensive approach known today as CBT.
Over the years, CBT has adapted and expanded to address a wider range of mental health issues, including anxiety disorders, depression, post-traumatic stress disorder (PTSD), and substance abuse. Research continually refines CBT techniques, leading to specialized forms tailored to specific populations and conditions.
Comparison of CBT with Other Therapeutic Approaches
CBT differs from other therapeutic approaches in its emphasis on present-focused problem-solving and skill-building. Unlike psychodynamic therapy, which explores unconscious conflicts and past experiences, CBT primarily focuses on current thoughts, feelings, and behaviors. Compared to humanistic therapies, which emphasize self-acceptance and personal growth, CBT adopts a more directive and structured approach, teaching specific coping mechanisms and strategies. While mindfulness-based therapies share some similarities with CBT in their focus on present moment awareness, CBT differs in its active and structured approach to identifying and modifying maladaptive thoughts and behaviors.
For example, while mindfulness might involve observing a negative thought without judgment, CBT would actively challenge and reframe that thought. The choice between therapeutic approaches depends on individual needs and preferences, with some individuals benefiting from an integrated approach combining elements of different therapies.
Stress and Anxiety Management using CBT: Cognitive Behavioral Therapy (CBT)
Cognitive Behavioral Therapy (CBT) offers a powerful framework for understanding and managing stress and anxiety. Unlike some therapies that focus solely on past experiences, CBT emphasizes the present, targeting unhelpful thought patterns and behaviors that contribute to these conditions. By identifying and modifying these patterns, individuals can learn to regulate their emotional responses and build resilience against future stressors.CBT addresses stress and anxiety symptoms by challenging negative or distorted thinking patterns and replacing them with more balanced and realistic perspectives.
It also helps individuals develop coping mechanisms and behavioral strategies to manage stressful situations effectively. This approach empowers individuals to take an active role in their own mental well-being.
Identifying and Challenging Negative Thoughts
A core component of CBT for stress and anxiety involves identifying and challenging negative automatic thoughts (NATs). These are the quick, often unconscious, thoughts that pop into our heads in response to stressful situations. For example, someone might have the NAT “I’m going to fail this presentation” before a work presentation. CBT techniques help individuals recognize these NATs, examine the evidence supporting and contradicting them, and then reframe them into more balanced and helpful thoughts.
This process helps reduce the emotional intensity associated with the stressful event. For instance, the NAT might be reframed to “I’ve prepared well, and while there’s always a chance of some nervousness, I’m capable of handling this.”
Developing Coping Mechanisms
CBT equips individuals with practical coping strategies to manage stress and anxiety in daily life. These strategies can be categorized into cognitive and behavioral techniques.
Cognitive techniques focus on modifying thought patterns. Examples include:
- Cognitive Restructuring: Actively challenging and replacing negative thoughts with more realistic and positive ones.
- Mindfulness: Paying attention to the present moment without judgment, reducing overthinking about the past or future.
- Positive Self-Talk: Replacing self-criticism with self-compassion and encouragement.
Behavioral techniques focus on changing actions and reactions to stressful situations. Examples include:
- Relaxation Techniques: Practicing techniques like deep breathing, progressive muscle relaxation, or meditation to reduce physical tension associated with anxiety.
- Exposure Therapy: Gradually exposing oneself to feared situations or objects in a safe and controlled manner to reduce avoidance and anxiety.
- Behavioral Activation: Engaging in enjoyable activities to increase positive mood and reduce withdrawal.
A Step-by-Step Guide to Anxiety Reduction using CBT
This guide Artikels a basic approach to using CBT techniques for anxiety reduction. It’s important to note that individual needs vary, and professional guidance is recommended for optimal results.
- Identify Triggers and Symptoms: Keep a journal documenting situations that trigger anxiety and the physical and emotional symptoms you experience.
- Identify Negative Thoughts: When you experience anxiety, note the negative thoughts that accompany it. Write them down.
- Challenge Negative Thoughts: Ask yourself: What evidence supports this thought? What evidence contradicts it? What is a more balanced way of thinking about this situation?
- Develop Coping Strategies: Choose specific coping mechanisms from the list above that you feel will be most effective for you. Practice them regularly.
- Practice Self-Compassion: Be kind and understanding to yourself. Progress takes time and setbacks are normal.
- Seek Professional Help: If anxiety significantly impacts your daily life, seeking professional help from a therapist specializing in CBT is crucial.
Mindfulness Practices in CBT

Mindfulness, the practice of paying attention to the present moment without judgment, is increasingly integrated into Cognitive Behavioral Therapy (CBT). This integration stems from the recognition that mindful awareness can significantly enhance the effectiveness of core CBT techniques by fostering self-awareness, emotional regulation, and behavioral change. By cultivating present moment awareness, individuals can better identify and understand their thoughts, feelings, and bodily sensations, paving the way for more effective cognitive restructuring and behavioral experiments.Mindfulness enhances the effectiveness of CBT interventions by providing a practical method for interrupting maladaptive thought patterns and emotional responses.
Traditional CBT focuses on identifying and challenging negative thoughts. Mindfulness complements this by offering a way to observe these thoughts without immediately reacting to them, creating psychological space for more objective evaluation and response. This non-reactive observation reduces the emotional intensity associated with negative thoughts, making cognitive restructuring more accessible and effective. Furthermore, mindfulness practices can improve self-compassion, reducing the self-criticism often associated with mental health challenges, and fostering a more accepting and supportive internal dialogue.
Mindfulness Exercises in CBT
Several mindfulness exercises are readily incorporated into CBT. These exercises aim to cultivate present moment awareness and enhance self-regulation skills, directly supporting the goals of CBT. The consistent practice of these exercises builds the foundation for improved emotional regulation and cognitive control.
Body Scan Meditation
This exercise involves systematically bringing awareness to different parts of the body, noticing sensations without judgment. Individuals lie down comfortably and begin by focusing on the sensations in their toes, gradually moving their attention upwards through their body, noticing any tingling, warmth, or tension. The process promotes body awareness and helps individuals connect with physical sensations, often overlooked during periods of stress or anxiety.
This practice helps to ground individuals in the present moment, reducing the tendency to get lost in rumination or worry about the future. For example, a person experiencing anxiety might notice the tension in their shoulders and jaw, leading to a greater understanding of the physical manifestations of their anxiety.
Mindful Breathing
Mindful breathing involves focusing on the sensation of breath entering and leaving the body. Individuals can pay attention to the rise and fall of their chest or abdomen, noticing the temperature and flow of air. When the mind wanders, which is natural, the individual gently redirects their attention back to the breath. This simple exercise cultivates present moment awareness and helps to calm the nervous system.
For instance, during a panic attack, focusing on the breath can help regulate heart rate and reduce feelings of overwhelming anxiety. The rhythmic nature of the breath acts as an anchor, grounding the individual in the present and reducing the intensity of overwhelming emotions.
Mindful Movement
Mindful movement incorporates awareness of physical sensations during movement. This can involve activities like yoga, tai chi, or even a simple mindful walk. The focus is on paying attention to the sensations in the body as it moves, noticing the feeling of the feet on the ground, the stretch in the muscles, and the rhythm of the breath.
This enhances body awareness and connects the mind and body, reducing stress and promoting relaxation. For example, a person experiencing depressive symptoms might find that a mindful walk in nature, focusing on the feeling of the wind on their skin and the sounds of the environment, improves their mood and reduces feelings of lethargy.
Mental Health Advocacy and CBT

Cognitive Behavioral Therapy (CBT) plays a vital role not only in treating mental health conditions but also in promoting mental wellness on a broader scale. By empowering individuals with coping mechanisms and self-awareness, CBT equips them to actively participate in advocating for better mental healthcare access and reducing the stigma associated with mental illness. This advocacy, in turn, creates a more supportive and understanding environment for everyone.CBT’s effectiveness in fostering mental health advocacy stems from its core principles.
The therapy teaches individuals to identify and challenge negative thought patterns and behaviors that may hinder their ability to advocate for themselves. It also helps them develop assertive communication skills and strategies for navigating challenging situations, such as interacting with healthcare providers or addressing discrimination. This self-empowerment is crucial in effectively navigating the complexities of mental healthcare systems and promoting positive change.
CBT’s Contribution to Mental Health Awareness and Stigma Reduction
CBT directly addresses the stigma surrounding mental health by helping individuals understand their conditions from a rational perspective, rather than one fueled by fear or shame. Through CBT, individuals learn to recognize and challenge negative self-perceptions and societal biases, replacing them with more balanced and realistic views. This increased self-understanding and self-acceptance can lead to more open communication about mental health, fostering empathy and reducing stigma within their personal networks and communities.
The skills learned in CBT, such as effective communication and assertive expression, are directly applicable to engaging in public conversations about mental health, contributing to broader societal awareness and understanding. For instance, a person who has successfully used CBT to manage anxiety might feel more confident sharing their experiences and advocating for improved mental health services in their workplace or community.
Empowering Individuals to Advocate for Their Mental Health Needs
CBT provides individuals with practical tools to navigate the healthcare system and advocate for their specific needs. This includes learning how to effectively communicate with healthcare providers, express their preferences for treatment, and assert their rights within the healthcare setting. For example, CBT can help individuals articulate their needs clearly and concisely, understand their treatment options, and advocate for a collaborative treatment plan tailored to their individual circumstances.
The therapy also helps individuals develop strategies for coping with potential setbacks or challenges they may encounter while navigating the healthcare system, such as insurance issues or bureaucratic hurdles. This proactive approach ensures that individuals are actively involved in their care, rather than passively accepting whatever is offered.
Examples of Successful Mental Health Advocacy Initiatives Utilizing CBT Principles, Cognitive behavioral therapy (CBT)
Several successful mental health advocacy initiatives have implicitly or explicitly incorporated CBT principles. Many peer support groups, for example, utilize elements of CBT by encouraging members to share their experiences, challenge negative thoughts, and develop coping strategies in a supportive environment. These groups provide a platform for individuals to learn from each other, build confidence, and collectively advocate for policy changes that benefit the mental health community.
Similarly, some public awareness campaigns utilize CBT-informed messaging to challenge negative stereotypes and promote a more compassionate understanding of mental illness. These campaigns often emphasize the importance of seeking help, normalizing mental health challenges, and highlighting the effectiveness of treatments like CBT. For instance, a campaign might feature testimonials from individuals who have successfully used CBT to manage their conditions, demonstrating the real-world impact of the therapy and encouraging others to seek help.
Therapy and Counseling Options incorporating CBT
Cognitive Behavioral Therapy (CBT) is a powerful tool, but its applications extend beyond standalone therapy. Many other therapeutic approaches integrate CBT techniques to enhance their effectiveness and provide a more comprehensive treatment plan for various mental health concerns. Understanding these integrated approaches is crucial for individuals seeking the right therapeutic fit.
Several therapeutic modalities successfully incorporate CBT principles. These approaches leverage CBT’s strengths in identifying and modifying maladaptive thoughts and behaviors while simultaneously addressing other crucial aspects of the individual’s experience, such as emotional regulation, interpersonal dynamics, and past trauma.
Dialectical Behavior Therapy (DBT)
DBT is specifically designed for individuals experiencing intense emotions and difficulties with self-harm or suicidal thoughts, often associated with borderline personality disorder. It integrates CBT’s focus on cognitive restructuring and behavioral skills training with mindfulness practices and acceptance-based strategies. This combination helps individuals manage their emotions, improve their relationships, and reduce self-destructive behaviors. DBT’s effectiveness is well-documented in treating borderline personality disorder and other conditions characterized by emotional dysregulation.
For example, studies have shown significant reductions in suicidal ideation and self-harm behaviors among individuals participating in DBT.
Acceptance and Commitment Therapy (ACT)
ACT focuses on accepting difficult thoughts and feelings rather than trying to control or eliminate them. While it shares CBT’s emphasis on behavioral change, it prioritizes identifying and pursuing one’s values. CBT techniques like cognitive defusion (distancing oneself from thoughts) are frequently used in ACT to help individuals experience thoughts and emotions without being overwhelmed by them. ACT’s effectiveness is particularly notable in treating anxiety, depression, and chronic pain.
For instance, research suggests ACT can significantly improve quality of life for individuals with chronic pain by helping them focus on valued activities despite their pain.
Cognitive Processing Therapy (CPT)
CPT is specifically tailored for trauma survivors. It combines CBT techniques with a focus on processing traumatic memories and their impact on current thinking and behavior. This approach helps individuals understand how their traumatic experiences shape their beliefs and behaviors, enabling them to challenge unhelpful thoughts and develop coping mechanisms. CPT is shown to be highly effective in treating PTSD, reducing symptoms such as intrusive thoughts, nightmares, and avoidance behaviors.
A study conducted by the Department of Veterans Affairs demonstrated significant improvements in PTSD symptoms among veterans undergoing CPT.
Guide for Individuals Seeking Therapy Incorporating CBT
Choosing the right therapy is a personal journey. When seeking therapy that incorporates CBT, it’s beneficial to:
- Clearly articulate your needs and goals to potential therapists.
- Inquire about their experience with CBT and related modalities.
- Consider your personal preferences and comfort level with different therapeutic approaches.
- Seek therapists with proven expertise and positive client testimonials.
- Engage in the initial consultation process to assess therapist-client fit.
Remember, finding the right therapist is a crucial step in your journey towards improved mental well-being. The collaborative nature of therapy ensures that the chosen approach aligns with your specific needs and preferences.
Cognitive behavioral therapy (CBT) stands as a remarkable testament to the power of understanding the mind-body connection. By equipping individuals with actionable strategies to identify and modify negative thought patterns and behaviors, CBT provides a pathway to improved mental health and enhanced personal well-being. Whether tackling stress, anxiety, depression, or addiction, CBT offers a practical and effective approach to cultivating resilience, fostering self-awareness, and ultimately, leading a more fulfilling life.
The journey to mental well-being is a personal one, and CBT provides the tools and support to navigate this journey successfully.
FAQ Compilation
How long does CBT therapy typically last?
The duration of CBT varies depending on individual needs and goals. Some individuals may benefit from a short-term course, while others may require longer-term treatment.
Is CBT right for everyone?
While CBT is highly effective for many, it may not be suitable for everyone. Individuals with severe mental illness or those who are not ready to actively participate in the therapeutic process may not find CBT as beneficial.
Can I do CBT on my own?
While self-help resources and books can provide an introduction to CBT principles, working with a trained therapist is generally recommended for optimal results. A therapist can provide personalized guidance and support.
What are the potential side effects of CBT?
CBT generally has few side effects. Some individuals may experience temporary emotional discomfort as they confront difficult thoughts and feelings during the therapy process.
How much does CBT cost?
The cost of CBT varies depending on the therapist, location, and insurance coverage. Some resources offer low-cost or sliding-scale options.





